Rare disease, common struggles: quality of life, caregiver burden and financial wellbeing of family caregivers in Poland
Rare diseases (RDs) are defined in Europe as life-threatening or chronically debilitating conditions affecting fewer than 1 in 2,000 people1,2. Some are even rarer, with ultra-rare diseases affecting fewer than 1 in 100,000 and hyper-rare fewer than 1 in 1,000,000. With over 10,000 identified RDs, they affect up to 30 million people in the EU, over 350 million globally, and an estimated 2.5 to 3 million individuals in Poland. Although RDs differ significantly in terms of etiology, epidemiology, symptoms, clinical progression, and prognosis – making direct comparisons challenging – they share several common characteristics that justify studying them collectively. Notably, 80% of RDs have a genetic origin, and 65% lead to serious clinical manifestations. Half of those affected by RDs are children, and tragically, 30% of children with a RDs do not survive past the age of five. Moreover, 95% of RDs currently lack an approved treatment, which adds to the medical and psychosocial burden experienced by affected families3.
RDs encompass a wide spectrum of conditions, including neurological, metabolic, and genetic disorders, each associated with distinct caregiving challenges. Neurological disorders, such as Dravet or Angelman syndrome, affect the brain, spinal cord, and nerves. They may be genetic, acquired, or idiopathic, and often involve seizures, cognitive decline, or motor impairments, requiring constant supervision and specialized rehabilitation4,5. Metabolic disorders, including phenylketonuria (PKU), Gaucher disease, or maple syrup urine disease, impair the body’s ability to process nutrients and energy. These conditions, often inherited, demand strict dietary control and continuous monitoring to prevent serious complications6,7. Genetic disorders result from mutations in DNA, either inherited or spontaneous. Conditions such as cystic fibrosis or muscular dystrophy typically affect multiple systems, cause lifelong disabilities, and require complex, multidisciplinary care8. These diverse conditions place significant emotional, physical, and logistical strain on caregivers, demanding intensive care, continuous learning, and frequent navigation of fragmented health and social systems.
While current research demonstrates decreased health-related quality of life and increased caregiving burden of parents of children with RDs, rare disease caregiving is associated with numerous adverse effects, thus clear definitions of key constructs are essential.
World Health Organization (WHO) defines quality of life (QoL) as an individual’s subjective assessment of their well-being, functioning, and satisfaction across various domains, including physical, emotional, and social aspects. This evaluation is influenced by personal goals, cultural background, and environmental context9.
Caregiver burden (CB), defined as a multidimensional response to stress and negative appraisal related to caregiving, negatively affects caregivers’ physical, emotional, and psychological health, lowering the QoL for both caregivers and children with RDs10. It includes both objective aspects (the time, physical effort and finances devoted to care) and subjective dimensions (emotional perception and experience). Importantly, the caregiver’s perception of the child’s symptoms and burden may be more significant than the medical diagnosis itself11,12.
One commonly accepted understanding of well-being describes it as a combination of individuals’ emotional experiences, their ability to manage daily life personally and socially, and their overall assessment of life satisfaction13.
Caring for individuals with RDs poses complex and multifaceted challenges, with a profound impact on caregivers’ QoL14,15,16,17,18. These challenges span emotional, physical, social, and financial domains. Prior research has consistently shown that caregiving burdens – including the financial strain of care19 and the uncertainty of the diagnostic odyssey20 – negatively affect caregivers’ mental and physical health, reduce social connectedness, and limit work productivity and overall well-being.
Emotional and social impacts are especially prominent. Caregivers frequently report anxiety, depression, guilt, and anticipatory grief17,18. Parents often describe emotional distress, severe emotional exhaustion and feelings of helplessness21,22,23. Socially, their participation in relationships and leisure activities often diminishes, while financial pressures arise due to reduced employment and increased healthcare expenses24,25. Despite these burdens, many caregivers also describe their roles as meaningful, suggesting a complex dynamic between strain and fulfillment.
Several factors influence CB, such as the severity and type of the child’s illness, caregiving duration, and caregiver demographics17,18. The burden of caregiving may also differ significantly between rare conditions, as highlighted in comparative studies of syndromes like Lennox-Gastaut and tuberous sclerosis complex22,26. Among these, financial well-being has emerged as a key moderating factor. It shapes how caregiving demands affect QoL across its physical, psychological, social, and environmental dimensions24,25. Financial security enables better access to services, improves emotional resilience, and enhances caregivers’ ability to maintain social ties and personal goals.
The practical demands of caregiving are substantial. Daily responsibilities often include managing complex medical regimens, liaising with multiple healthcare providers, and arranging emotional and social support27. Limited access to formal support systems and respite services compounds caregivers’ stress28which may result in physical exhaustion and a sense of social isolation29. Additionally, caregivers are especially vulnerable to “financial toxicity”, a condition where limited resources lead to heightened stress and forced trade-offs in treatment and care30.
The diagnostic odyssey adds further strain. Caregivers commonly face delayed, incomplete, or incorrect diagnoses, which prolong uncertainty, hinder access to appropriate therapies, and increase both emotional and financial costs31,32. Misdiagnoses often lead to unnecessary procedures and emotional distress33. Encounters with clinicians unfamiliar with RDs can also leave families feeling unsupported17,18,29.
Financial well-being plays a crucial protective role. Caregivers with greater economic resources typically enjoy better access to healthcare and support networks, which bolster coping strategies and QoL34. It helps alleviate stress, facilitates participation in socially and emotionally enriching activities, and improves caregivers’ overall resilience.
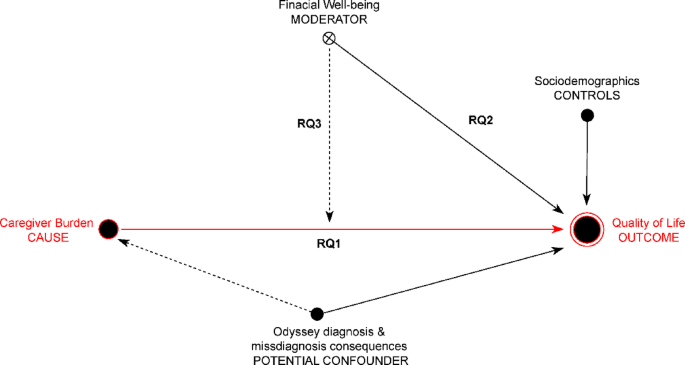
This study investigates the moderating role of financial well-being in the relationship between CB and QoL across four dimensions: physical health, psychological health, social relationships, and environment. Guided by a theoretical model (Fig. 1), we aim to address the following research questions:
RQ1
How does CB influence QoL, and does this effect vary across different QoL dimensions?
RQ2
What is the direct effect of financial well-being on caregivers’ QoL across the four domains?
RQ3
Does financial well-being moderate the relationship between CB and QoL?
The findings aim to inform the development of targeted interventions to alleviate CB and improve caregivers’ QoL, particularly by addressing financial challenges and enhancing support systems.
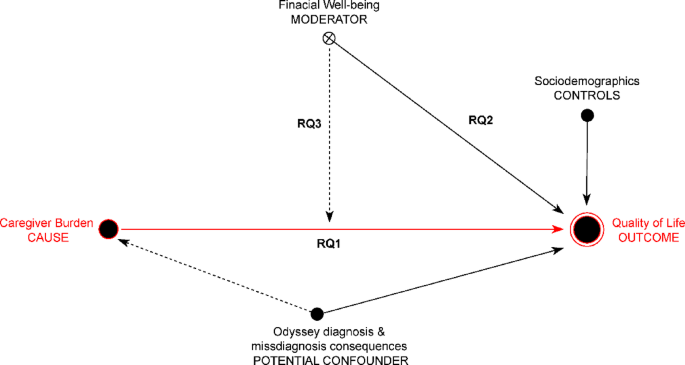
A theoretical model for examining the moderating effect of financial well-being on the impact of caregiver burden on perceived quality of life.
link







