Effects of meteorological factors and air pollution on the number of allergic rhinitis outpatient visits in Changchun city, China
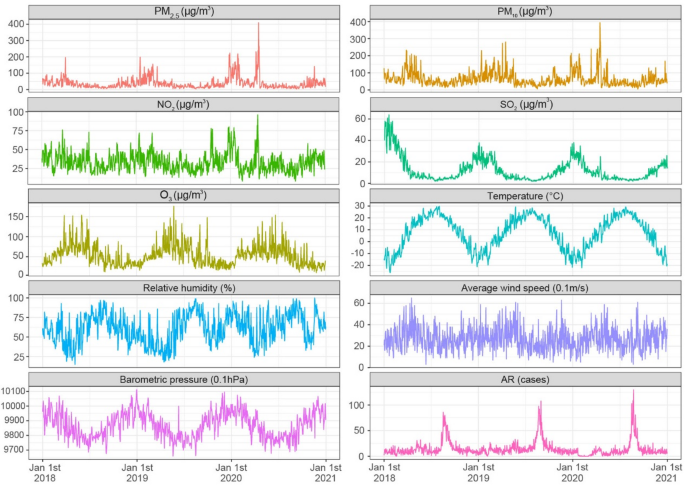
In this study, by analyzing the association between air pollutants, meteorological factors, and the number of AR outpatient visits in Changchun City from 2018 to 2020, we found a positive correlation between increasing pollutant concentrations (PM2.5, PM10, NO2, and SO2) and the number of AR outpatient visits. Non-linear correlations were found between temperature, RH, average wind speed, barometric pressure and the number of AR outpatient visits. Among the extreme meteorological factors, low and high temperatures, low RH and low barometric pressure have hazardous effects on patients with AR. The effects of extreme meteorological factors were more pronounced in those aged < 15 years. And the effects of air pollution on the number of AR outpatient visits were enhanced at low temperatures and RHs. Air pollution and meteorological changes increase the risk of AR morbidity. Therefore, more attention should be paid to the impact of air pollution and meteorological factors on public health.
The onset of AR is correlated with both innate genetic background and acquired environmental factors, and air pollution is a major environmental risk factor for the increased incidence of AR21,22. In this study, we found positive correlations between PM2.5, PM10, NO2, SO2, and the number of AR outpatient visits, and there were immediate and cumulative lagged effects on AR onset, and the single-day lagged effects of the pollutants were maximum on the day of exposure. For every 10 µg/m3 increase in the daily average pollutant concentration of PM2.5, PM10, and NO2, and per 1 µg/m3 increase in the daily average concentration of SO2, the number of AR outpatient visits increased by 1.45%, 1.03%, 3.98%, and 1.68%, respectively, and this result was consistent with those of other urban studies14,16,18,21,23. An Australian study found that the severity of AR symptoms and PM were correlated24. However, a long-term study did not find a significant correlation between PM2.5, NO2, and O3 and AR25. Atkinson et al.26 found that O3 has adverse effects on the respiratory system and may increase the risk of asthma and AR onset, and that the concentration of O3 was positively correlated with the prevalence of AR21. However, O3 had no effect on childhood AR development27. In our study, O3 did not have a significant impact on the number of AR clinic visits. Few studies have been conducted on the harmful effects of O3; therefore, further research is required. The differences between the results of these studies may be due to differences in study populations, study sizes, geographic location, and duration of air pollution28.
The exact mechanism underlying the association between air pollutants and AR has not been strongly demonstrated, and its possible mechanisms are that air pollution aggravates inflammation, promotes oxidative stress, interferes with signal transduction, and leads to immunosuppression, enzyme inhibition, and epigenetic dysregulation29,30,31,32. Ackaert et al.33 found that air pollutants can directly affect the immune system and induce oxidative stress or inflammation. Activated trace gases, such as O3 and NO2, can induce post-transformation modifications, thereby changing the immunogenicity of proteins. Inhalation of air pollutants such as PM, NO2, SO2, and O3 may impair the nasal mucosa and the clearing function of the nasal mucosal cilia, which can damage the immune system34. Air pollutants may contribute to AR pathogenesis by damaging the nasal mucosa, inducing inflammation of the nasal airways, stimulating the synthesis of IgE antibodies, and sensitizing the airways to allergens15. Owing to the complex etiology of AR, the pathophysiological mechanisms underlying the effects of air pollution on AR need to be further explored.
Climate change is widely recognized as the greatest challenge to global health in the 21st century35,36, and in this study, we found that, under extreme meteorological conditions, low and high temperatures, low RH and lower barometric pressure had hazardous effects. The stimulation of temperature changes, especially low temperatures37 can promote the release of neurotransmitters and increase secretion from nasal glands and vascular permeability, thus promoting the onset of AR10,38. In addition, ambient temperature can alter vegetation patterns in space and time and affect allergic symptoms in several ways, thus indirectly affecting AR onset39,40. Combined with the climate characteristics of Changchun, the increased risk of AR incidence from December to January in Changchun may be related to the effect of temperature. We will follow up with patients with AR to comprehensively investigate whether low temperatures exacerbate AR symptoms. Men are more susceptible to temperature changes than women9,10,41, and in our study, female were more sensitive to high temperatures, considering that it is related to the differences in physiological mechanisms between men and women. Children with AR were more vulnerable to the effects of low temperatures compared to other age groups.
Studies in different regions have found that both high and low RHs can be potential risk factors for an increased incidence of AR11,42,43. Low humidity conditions may favor allergen transmission by causing nasal mucosal damage and reducing the barrier effect of the nasal mucosa against allergens11, whereas high RH favors allergen growth and multiplication44. However, at high RH, the moisture mass of the pollen increases, and the particles become larger and less easily dispersed. Combined with the results of our study, the greater effect of low RHs on AR onset in Changchun suggests that allergen release and diffusion may be high-risk factors for AR onset in Changchun.
We also found that low barometric pressure increases the incidence of allergic rhinitis. Previous studies have shown that low pressure is often accompanied by humid and rainy weather. High humidity environments can promote the growth of mold and dust mites, thereby increasing exposure to allergens45. Low pressure is also often associated with weakened air convection, which leads to the accumulation of pollutants and allergens near the ground, causing synergistic irritation of the respiratory tract.
In our study, compared with adults and the elderly, children were more sensitive to overall extreme meteorological factors. Low temperature, high RH, and low wind speed increased the number of AR outpatient visits in children, which may be related to the incomplete development of children’s immune systems and their weak adaptive ability to extreme meteorological conditions. The mechanism by which meteorological factors influence AR development in children has not yet been established, and further studies are needed.
Meteorological factors can act synergistically with air pollution to adversely affect human health46,47. Wu et al.14 found that the effect of air pollution on AR may be enhanced at low temperatures and high RHs in Beijing. In this study, we found that the effect of pollutants on AR onset is enhanced at low temperatures and RH in Changchun and that different air pollutants are affected differently by temperature and RH. The potential mechanisms by which temperature influences the effects of air pollution are unknown; however, it has been suggested that low temperatures increase the adverse effects of air pollutants on respiratory mucosal ciliary function, causing airway damage, which can lead to high airway sensitivity to air pollution48,49. Higher temperatures and sunlight intensity may accelerate the photochemical-induced aging of airborne particulate matter, thereby affecting the chemical properties of air pollution mixtures, photochemically formed secondary aerosols may be less toxic than their precursors50,51. However, few studies have investigated whether RH can modify the effects of air pollution on human health52. At a high RH, the air is more humid, and the size of airborne pollutant particles may increase owing to hygroscopicity, which may negatively affect the ease at which air pollutant particles are inhaled52,53. However, the mechanism underlying the interaction between meteorological factors and air pollution requires further study.
This study concluded that air pollution and meteorological factors are associated with the number of outpatient visits for AR, and attention should be paid to the impact of these factors on patients. Stronger environmental policies and public health interventions can be formulated to effectively reduce the incidence of AR, reduce the public health burden and improve public health. It also reminds healthcare professionals and patients to be aware of the impact of environmental factors on AR, to prepare in advance for resource allocation, diagnosis and treatment, and to help patients cope with the health risks associated with environmental changes by strengthening patient health education and developing targeted personal protective measures. The study also concluded that more attention should be paid to the impact of environmental change on children.
This study had limitations that must be acknowledged. First, pollutant-exposure data were derived from fixed-site detectors. This may have caused potential misclassification of exposures, leading to a bias toward the null hypothesis and an underestimation of the estimated effects. Second, the prevalence of AR showed significant geographic variation54; and as this was a single-center study conducted in Changchun City, the conclusions may not apply to other regions and should not be generalized to other geographic areas. Finally, owing to the lack of daily pollen level monitoring in our region, we were unable to assess the effect of pollen concentration on changes in the number of AR outpatient visits.
link





