Clinical characteristics and outcomes of COVID-19 in pediatric patients with rheumatic diseases
To our knowledge, this study is the first to comprehensively track the clinical symptoms within two weeks of COVID-19 infection in pediatric patients with rheumatic diseases in China. Our findings indicated that fever typically appeared within the first three days and was significantly negatively associated with all other symptoms and coughing persisted longer than other symptoms. Notably, vaccination was found to lower hospitalization risk and shorten the duration of negative conversion. Majority of participants had mild COVID-19 symptoms. Our results underscore the importance of monitoring a range of clinical symptoms that may positively correlate during the course of COVID-19 infection.
This study identified that fever, cough, runny nose, sore throat and other symptoms of upper respiratory tract infection as the most common manifestations of COVID-19 in pediatric patients during the epidemic period. These findings are consistent with a study conducted in New York on pediatric patients with rheumatic diseases, which also reported fever, fatigue, and cough as prevalent symptoms.10 Additionally, our results align with previous studies conducted on healthy children.11 Additionally, gastrointestinal symptoms, malaise, and irritability were observed, although they were less common and often not associated with the lower respiratory tract.
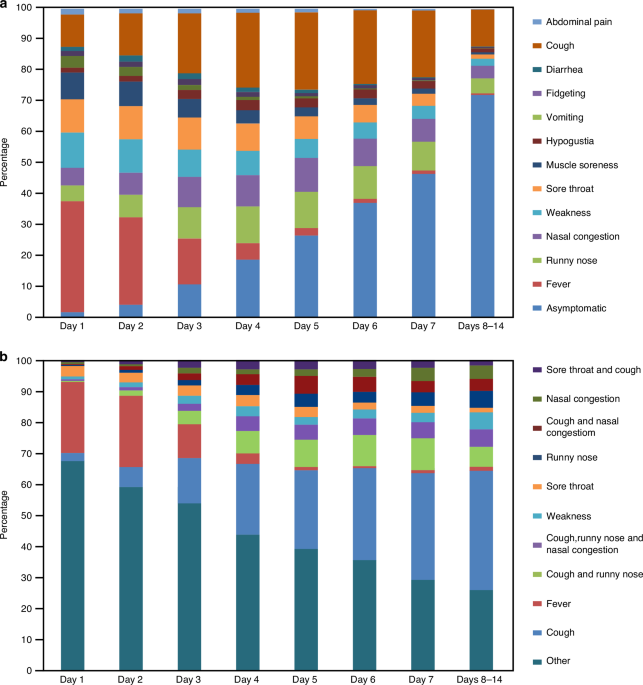
Regarding the correlation of symptoms, fever was the most prominent early symptom and typically the first to appear. As fever subsided, symptoms such as cough, nasal congestion, and runny nose became more prevalent, with cough being the longest-lasting symptom. The combination of cough and runny nose was the most frequent symptom pairing. Therefore, it is important to focus on fever in the initial 1–3 days of infection and on respiratory symptoms, which become more common after the fourth day. Prolonged cough may indicate potential lower respiratory tract involvement. A study from South Africa also found that fever (46%) and cough (40%) were the main symptoms in children infected with the Omicron variant.12 The prevalence of fever and cough in our study was significantly higher than in the South African study and previous reports,13,14 likely due to differences in virus strains. While loss of smell and taste was common in earlier COVID-19 infections, the prevalence of these symptoms decreased with the Omicron variant, with only 11.2% of children in our survey reporting loss of taste. In our cohort, approximately 2% of children were asymptomatic, a lower rate compared to the 12.9–38.9% reported in Western studies.8,15 This discrepancy may be due to differences in ethnicity, increased symptom burden from underlying rheumatic diseases, or the timing of nucleic acid or antigen testing, which may have missed asymptomatic cases. This discrepancy may be due to the difference in ethnics, increased symptom burden from underlying diseases or the timing of nucleic acid or antigen testing, which may have missed asymptomatic cases.
Pediatric patients with rheumatic diseases often receive immunosuppressive therapy, making them more susceptible to infections. However, previous research has shown that patients with rheumatoid arthritis or spondy loarthritis on biologic agents did not develop severe respiratory complications from COVID-19, suggesting these treatments may mitigate the abnormal inflammatory and cytokine responses that lead to severe disease.16 A similar study from Spain has suggested that treatment with glucocorticoids increases the risk of hospital admission due to COVID-19.15 Additionally, pediatric patients with childhood-onset systemic lupus erythematosus who are treated with rituximab therapy may face an increased risk of severe infections.17 A multicenter study involving 113 children with rheumatic diseases treated with multiple biologic disease-modifying antirheumatic drugs (bDMARDs) found no association between biologic therapy and adverse COVID-19 outcomes.18 Similarly, in our study, 45.51% of children were on bDMARDs, and we found that bDMARD use did not prolong the time to COVID-19 negativity. Conversely, corticosteroid use, including prednisone acetate (≥ 5 mg/d) and methylprednisolone (≥ 4 mg/d), was associated with a shorter time to COVID-19 negativity, likely due to reduced inflammatory activity, contrasting with previous findings that corticosteroids may prolong viral clearance.19 A Japanese study indicated that children with rheumatic diseases treated with traditional disease-modifying antirheumatic drugs (tDMARDs) did not show an elevated risk of contracting COVID-19 or experiencing severe outcomes from the disease.20 These data suggest that tDMARDs should be continued for these patients during a pandemic.7
The present study observed that 45 children (4.21%) with COVID-19 infection required hospital admission. This finding aligns with a study conducted in Turkey, which reported that children with rheumatic diseases did not have higher hospitalization rates for COVID-19 compared to their healthy counterparts.8 During the same period, the hospitalization rate for adult patients with rheumatic diseases in China was 5.29% (231 out of 4370), which is marginally higher than the rate observed in our study.21 In comparison, among Chinese pediatric patients in the fields of hematology and oncology—who are in a similarly immunocompromised state as our study population—8.17% (25 out of 306) required hospitalization following COVID-19 infection.22 This is consistent with findings from the United States, which demonstrated that symptomatic subjects with mild COVID-19 symptoms indicate minimal risk of severe or critical COVID-19 in immunosuppressed pediatric rheumatic disease patients.10
The pathogenesis of COVID-19 represents two distinct but overlapping phases of COVID-19 infection. The first phase is initiated by the virus itself, commencing when the infectious virus enters the respiratory tract and has the capability to infect alveolar cells through binding to angiotensin-converting enzyme 2 (ACE2) receptors, resulting in initial cold and flu-like symptoms.23 The elevated infection rate among children with the Omicron variant is associated with an increased binding affinity for the receptor-binding domain (RBD)-ACE2 complex of Omicron.24,25 One reason for the predominance of asymptomatic infections and milder disease severity among children with COVID-19 compared to adults may be related to the different immune profiles of the two. Compared to adults, the immune system of the upper respiratory mucosa in children is in a preactivated state and therefore can release interferons and control the infection early in COVID-19.14 In contrast, in adult COVID-19 patients, more robust adaptive immunity may instead lead to a dysregulated systemic inflammatory response resulting in multiorgan damage.26 Another explanation for the milder symptoms observed in children is their primary exposure to adult family members. Our data showed that family transmission was the primary mode of infection among children, accounting for 64.11% of cases, consistent with the findings of previous studies.27 Therefore, children may be infected with second- or third-generation viruses, potentially leading to a decrease in the pathogenicity of the strain [9]. Children infected with COVID-19 are still at risk of severe disease, the second stage of infection, the “cytokine storm”,23 which manifests as respiratory failure, myocarditis, shock, acute renal failure, coagulopathy, neurological involvement (encephalitis and stroke, cerebral edema, Guillain–Barre syndrome) and multisystem organ failure. While the occurrence is rare, a small percentage of children may develop a particularly severe condition called MIS-C after infection,28 a very concerning condition in children with COVID-19.
Our results indicated that vaccines may help reduce serious clinical outcomes among children with COVID-19. It has been reported that one of the advantages of COVID-19 vaccination is protection against long-term COVID-19 and its associated conditions, as well as a reduced risk of hospitalization.29,30 Our study consistently confirms that vaccination have positive impacts on children with rheumatic diseases. A study by Hu et al.31 showed that children who received vaccination from primary carers who had received more than two doses of a vaccine had shorter nucleic acid conversion times. Therefore, active vaccination of both eligible children and carers should be considered to reduce the risk of infection and disease in childhood cases within the family. Despite lower seropositivity rates for COVID-19 vaccination among patients with rheumatic diseases than in the general population,32 the European Alliance of Associations for Rheumatology (EULAR) recommends that all rheumatic patients, including those taking corticosteroids, methotrexate, bDMARDs or tDMARDs, should receive the COVID-19 vaccine.33,34
The results of the attribution analysis revealed that children with primary immunodeficiency had prolonged symptom durations compared to those with other rheumatic diseases. This can be attributed to their low autoimmune function and compromised ability to clear viruses. On the other hand, younger children may exhibit shorter durations of symptoms due to their limited ability to express their feelings effectively. Additionally, the shorter symptom durations observed in children treated with prednisone can be attributed to the use of glucocorticoids, which reduce the inflammatory response following an infection.
This study has several limitations. First, we did not include a control group of healthy children with COVID-19 for comparison. The children admitted to the hospital often had severe symptoms, which may have introduced selection bias, as these children are not representative of the general pediatric population. Second, the scope of symptoms evaluated was limited. The questionnaire relied on self-reporting by families, which could have resulted in incomplete information and subjective differences in symptom interpretation. Third, the questionnaire was not distributed in intensive care units, emergency departments, or other high-prevalence severe illness areas, leading to a potential underrepresentation of more severe cases of COVID-19. Furthermore, because we did not differentiate between active and inactive disease status for diseases known to have a prolonged course (e.g., juvenile idiopathic arthritis, systemic lupus erythematosus) versus monophasic diseases (e.g., Henoch-Schonlein purpura). Those with inactive disease may have experienced milder symptoms of COVID-19, might contributing to potential bias in the study findings, despite of the majority of the participants have chronic rheumatic diseases.
In summary, this study is the first to provide data on COVID-19 infection in children with rheumatic diseases in China, shedding light on the clinical and epidemiological characteristics of the disease in this demographic. The results indicate that the current wave of COVID-19 infections in this population has been mild, predominantly manifesting as upper respiratory symptoms. This study not only raises awareness regarding the health outcomes for children with rheumatic diseases who contract COVID-19 but also offers guidance on the use of medications for their primary condition. The findings highlight the importance of promoting vaccination against COVID-19 in this vulnerable population. Further studies are needed to explore the long-term effects of COVID-19 on children with rheumatic diseases.
link







