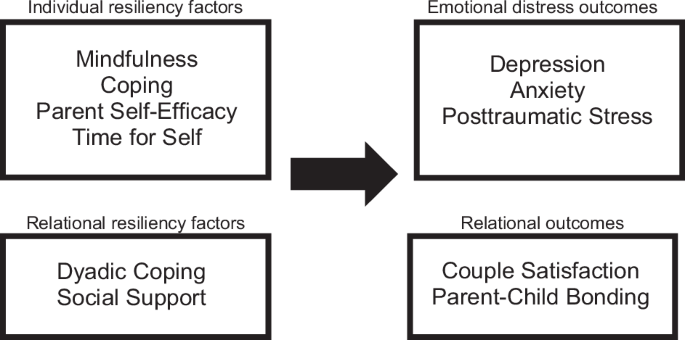
Resiliency factors relevant to NICU parents’ emotional and relational health
Harrison W, Goodman D. Epidemiologic trends in neonatal intensive care, 2007-2012. JAMA Pediatr. 2015;169:855–62.
Malouf R, Harrison S, Burton HAL, Gale C, Stein A, Franck LS, et al. Prevalence of anxiety and post-traumatic stress (PTS) among the parents of babies admitted to neonatal units: a systematic review and meta-analysis. EClinicalMedicine. 2022;43:101233. https://doi.org/10.1016/j.eclinm.2021.101233.
Google Scholar
Scarff JR. Postpartum depression in men. Innov Clin Neurosci. 2019;16:11–14.
Google Scholar
Gerstein ED, Njoroge WFM, Paul RA, Smyser CD, Rogers CE. Maternal depression and stress in the neonatal intensive care unit: associations with mother-child interactions at age 5 years. J Am Acad Child Adolesc Psychiatry. 2019;58:350–8.e2. https://doi.org/10.1016/j.jaac.2018.08.016.
Google Scholar
Bozkurt O, Eras Z, Sari FN, Dizdar EA, Uras N, Canpolat FE, et al. Does maternal psychological distress affect neurodevelopmental outcomes of preterm infants at a gestational age of ≤32weeks. Early Hum Dev. 2017;104:27–31. https://doi.org/10.1016/j.earlhumdev.2016.11.006.
Google Scholar
Ferrand A, Gorgos A, Ali N, Payot A. Resilience rather than medical factors: how parents predict quality of life of their sick newborn. J Pediatr. 2018;200:64–70.e5. https://doi.org/10.1016/j.jpeds.2018.05.025.
Google Scholar
Ivashchuk A, Guillen U, Mackley A, Locke R, Sturtz W. Parental protective factors and stress in NICU mothers and fathers. J Perinatol. 2021;41:2000–8. https://doi.org/10.1038/s41372-020-00908-4.
Google Scholar
Rossman B, Greene MM, Kratovil AL, Meier PP. Resilience in mothers of very-low-birth-weight infants hospitalized in the NICU. J Obstet Gynecologic Neonatal Nurs. 2017;46:434–45. https://doi.org/10.1016/j.jogn.2016.11.016.
Google Scholar
Herrman H, Stewart DE, Diaz-Granados N, Berger EL, Jackson B, Yuen Tracy. What is resilience?. Can J Psychiatry. 2011;56:258–65. https://doi.org/10.1177/070674371105600504.
Google Scholar
Brown KW, Ryan RM. The benefits of being present: mindfulness and its role in psychological well-being. J Personal Soc Psychol. 2003;84:822–48. https://doi.org/10.1037/0022-3514.84.4.822.
Google Scholar
Gamarel KE, Revenson TA. Dyadic adaptation to chronic illness: the importance of considering context in understanding couples’ resilience. In: Couple resilience: emerging perspectives. Springer Science + Business Media; 2015. pp. 83–105. https://doi.org/10.1007/978-94-017-9909-6_5
Folkman S, Lazarus RS. An analysis of coping in a middle-aged community sample. J Health Soc Behav. 1980;21:219–39. https://doi.org/10.2307/2136617.
Google Scholar
Lim Jwon, Shon Ejung, Paek M, Daly B. The dyadic effects of coping and resilience on psychological distress for cancer survivor couples. Support Care Cancer. 2014;22:3209–17. https://doi.org/10.1007/s00520-014-2334-9.
Google Scholar
Falconier MK, Kuhn R. Dyadic coping in couples: a conceptual integration and a review of the empirical literature. Front Psychol. 2019;10:571. https://doi.org/10.3389/fpsyg.2019.00571.
Google Scholar
García-Martín MÁ, Hombrados-Mendieta I, Gómez-Jacinto L. A multidimensional approach to social support: the questionnaire on the frequency of and satisfaction with social support (QFSSS). Anales Psicol. 2016;32:501. https://doi.org/10.6018/analesps.32.2.201941.
Google Scholar
Vranceanu AM, Bannon S, Mace R, Lester E, Meyers E, Gates M, et al. Feasibility and efficacy of a resiliency intervention for the prevention of chronic emotional distress among survivor-caregiver dyads admitted to the neuroscience intensive care unit: a randomized clinical trial. JAMA Netw Open. 2020;3:e2020807 https://doi.org/10.1001/jamanetworkopen.2020.20807.
Google Scholar
McCubbin H, Olson DH, Patterson JM. Beyond family crisis: family adaptation. Int J Mass Emerg Disasters. 1983;1:73–93.
Google Scholar
Grunberg VA, Geller PA, Hoffman C, Patterson CA. A biopsychosocial model of NICU family adjustment and child development. J Perinatol. 2023;43:510–7. https://doi.org/10.1038/s41372-022-01585-1.
Google Scholar
Grunberg VA, Geller PA, Patterson CA. Infant illness severity and family adjustment in the aftermath of NICU hospitalization. Infant Ment Health J. 2020;41:340–55. https://doi.org/10.1002/imhj.21848.
Google Scholar
Grunberg VA, Presciutti A, Vranceanu AM, Lerou PH. Parental self-efficacy and personal time help explain impact of parent-staff interactions on parental distress and bonding in the neonatal intensive care unit. J Pediatr. 2025;276:114300. https://doi.org/10.1016/j.jpeds.2024.114300.
Google Scholar
Self-efficacy in changing societies. Cambridge University Press; 1995:xv, 334. https://doi.org/10.1017/CBO9780511527692.
Vance AJ, Pan W, Malcolm WH, Brandon DH. Development of parenting self-efficacy in mothers of high-risk infants. Early Hum Dev. 2020;141:104946. https://doi.org/10.1016/j.earlhumdev.2019.104946.
Google Scholar
Garfield CF, Kerrigan E, Christie R, Jackson KL, Lee YS. A mobile health intervention to support parenting self-efficacy in the neonatal intensive care unit from admission to home. J Pediatr. 2022;244:92–100. https://doi.org/10.1016/j.jpeds.2022.01.004.
Google Scholar
Gómez-Cantarino S, García-Valdivieso I, Moncunill-Martínez E, Yáñez-Araque B, Ugarte Gurrutxaga MI. Developing a family-centered care model in the neonatal intensive care unit (NICU): a new vision to manage healthcare. Int J Environ Res Public Health. 2020;17:7197 https://doi.org/10.3390/ijerph17197197.
Google Scholar
Hill C, Knafl KA, Santacroce SJ. Family-centered care from the perspective of parents of children cared for in a pediatric intensive care unit: an integrative review. J Pediatr Nurs. 2018;41:22–33. https://doi.org/10.1016/j.pedn.2017.11.007.
Google Scholar
Franck LS, O’Brien K. The evolution of family-centered care: from supporting parent-delivered interventions to a model of family integrated care. Birth Defects Res. 2019;111:1044–59. https://doi.org/10.1002/bdr2.1521.
Google Scholar
Onken LS, Carroll KM, Shoham V, Cuthbert BN, Riddle M. Reenvisioning clinical science: unifying the discipline to improve the public health. Clin Psychol Sci. 2014;2:22–34. https://doi.org/10.1177/2167702613497932.
Google Scholar
Cuschieri S. The STROBE guidelines. Saudi J Anaesth. 2019;13:S31–S34. https://doi.org/10.4103/sja.SJA_543_18.
Google Scholar
Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67:361–70. https://doi.org/10.1111/j.1600-0447.1983.tb09716.x.
Google Scholar
Dagnan D, Chadwick P, Trower P. Psychometric properties of the Hospital Anxiety and Depression Scale with a population of members of a depression self-help group. Br J Med Psychol. 2000;73:129–37. https://doi.org/10.1348/000711200160255.
Google Scholar
Hagen IH, Svindseth MF, Vasset FP. Association between parents’ perceived mental distress and support and satisfaction in neonatal intensive care units. Klin Sygepleje. 2023;37:19–33. https://doi.org/10.18261/ks.37.1.3.
Google Scholar
Bjelland I, Dahl AA, Haug TT, Neckelmann D. The validity of the Hospital Anxiety and Depression Scale. Update Lit Rev J Psychosom Res. 2002;52:69–77. https://doi.org/10.1016/s0022-3999(01)00296-3.
Google Scholar
Thoresen S, Tambs K, Hussain A, Heir T, Johansen VA, Bisson JI. Brief measure of posttraumatic stress reactions: impact of Event Scale-6. Soc Psychiat Epidemiol. 2010;45:405–12. https://doi.org/10.1007/s00127-009-0073-x.
Google Scholar
Hosey MM, Leoutsakos JMS, Li X, Dinglas VD, Bienvenu OJ, Parker AM, et al. Screening for posttraumatic stress disorder in ARDS survivors: validation of the Impact of Event Scale-6 (IES-6). Crit Care. 2019;23:276. https://doi.org/10.1186/s13054-019-2553-z.
Google Scholar
Jeong J, Kim AR, Hilton C, Hong I. Impact of Event Scale-6 (IES-6) for U.S. adults who experienced the COVID-19 pandemic. BMC Psychiatry. 2022;22:490. https://doi.org/10.1186/s12888-022-04136-2.
Google Scholar
Ionio C, Colombo C, Brazzoduro V, Mascheroni E, Confalonieri E, Castoldi F, et al. Mothers and fathers in NICU: the impact of preterm birth on parental distress. Eur J Psychol. 2016;12:604–21. https://doi.org/10.5964/ejop.v12i4.1093.
Google Scholar
Funk JL, Rogge RD. Testing the ruler with item response theory: increasing precision of measurement for relationship satisfaction with the Couples Satisfaction Index. J Fam Psychol. 2007;21:572–83. https://doi.org/10.1037/0893-3200.21.4.572.
Google Scholar
Schwenck GC, Dawson SJ, Allsop DB, Rosen NO. Daily dyadic coping: associations with postpartum sexual desire and sexual and relationship satisfaction. J Soc Personal Relatsh. 2022;39:3706–27. https://doi.org/10.1177/02654075221107393.
Google Scholar
Brockington IF, Oates J, George S, Turner D, Vostanis P, Sullivan M, et al. A screening questionnaire for mother-infant bonding disorders. Arch Womens Ment Health. 2001;3:133–40. https://doi.org/10.1007/s007370170010.
Google Scholar
Ettenberger M, Bieleninik Ł, Stordal AS, Ghetti C. The effect of paternal anxiety on mother-infant bonding in neonatal intensive care. BMC Pregnancy Childbirth. 2024;24:55. https://doi.org/10.1186/s12884-023-06179-z.
Google Scholar
Feldman G, Hayes A, Kumar S, Greeson J, Laurenceau JP. Mindfulness and emotion regulation: the development and initial validation of the cognitive and affective mindfulness scale-revised (CAMS-R). J Psychopathol Behav Assess. 2007;29:177–90. https://doi.org/10.1007/s10862-006-9035-8.
Google Scholar
Marshall A, Guillén Ú, Mackley A, Sturtz W. Mindfulness Training among parents with preterm neonates in the neonatal intensive care unit: a pilot study. Am J Perinatol. 2019;36:1514–20. https://doi.org/10.1055/s-0039-1678557.
Google Scholar
Antoni MH, Lechner SC, Kazi A, Wimberly SR, Sifre T, Urcuyo KR, et al. How stress management improves quality of life after treatment for breast cancer. J Consulting Clin Psychol. 2006;74:1143–52. https://doi.org/10.1037/0022-006X.74.6.1143.
Google Scholar
Psychometric properties of the Measurement of Current Status (MOCS) Scale in Mexican cancer patients. 2024. Accessed November 8, 2024.
Riklin E, Calandrillo D, Blitz A, Zuckerberg D, Annunziato RA. Examining the psychosocial needs of adolescents with craniofacial conditions: a mixed-methods approach. Cleft Palate Craniofacial J. 2020;57:177–85. https://doi.org/10.1177/1055665619870621.
Google Scholar
Meyers EE, Presciutti A, Shaffer KM, Gates M, Lin A, Rosand J, et al. The impact of resilience factors and anxiety during hospital admission on longitudinal anxiety among dyads of neurocritical care patients without major cognitive impairment and their family caregivers. Neurocrit Care. 2020;33:468–78. https://doi.org/10.1007/s12028-020-00913-7.
Google Scholar
Bodenmann G. Dyadisches coping inventar [dyadic coping inventory]. Manual. Bern Huber. – References – Scientific Research Publishing; 2008. Accessed December 8, 2025.
Roth M, Weitkamp K, Landolt SA, Bodenmann G. Couples’ dyadic coping in the context of child-related stressors: A systematic review across three decades. Couple Fam Psychol Res Pract. 2024;13:202–23. https://doi.org/10.1037/cfp0000237.
Google Scholar
Başgöl Ş, Koç E, Çankaya S. The relationship between postpartum mothers’ dyadic coping and adjustment and psychological well-being. Curr Psychol. 2024;43:20668–76. https://doi.org/10.1007/s12144-024-05844-6.
Google Scholar
Parenting Sense Of Competence Scale (PSOC). 2021. Accessed December 8, 2025.
Ohan JL, Leung DW, Johnston C. The Parenting Sense of Competence scale: Evidence of a stable factor structure and validity. Can J Behav Sci Rev Canadienne Des Sci Du Comport. 2000;32:251–61. https://doi.org/10.1037/h0087122.
Google Scholar
Huang L, Wang XJ, Liu GH, Li XT, Zhang YH, Zhao BY, et al. Parenting sense of competence among chinese parents of premature infants: a cross-sectional study. BMC Pregnancy Childbirth. 2023;23:399. https://doi.org/10.1186/s12884-023-05703-5.
Google Scholar
Khodabandeh Shahraki S, Bazyar M, Nematollahi M, Emadi SF, Tavan A. Impact of family-centered care on parenting role and sense of competence in parents of preterm neonates: a quasi-experimental study. J Neonatal Nurs. 2025;31:267–74. https://doi.org/10.1016/j.jnn.2024.08.012.
Google Scholar
Van Horn ML, Bellis JM, Snyder SW. Family resource scale-revised: psychometrics and validation of a measure of family resources in a sample of low-income families. J Psychoeducational Assess. 2001;19:54–68. https://doi.org/10.1177/073428290101900104.
Google Scholar
Zimet GD, Dahlem NW, Zimet SG, Farley GK. The multidimensional scale of perceived social support. J Personal Assess. 1988;52:30–41. https://doi.org/10.1207/s15327752jpa5201_2.
Google Scholar
Erbaba H, Pinar G. Association of perceived social support and maternal adaptation with postpartum depression in mothers of infants hospitalized in neonatal intensive care units. J Neonatal Nurs. 2021;27:251–6. https://doi.org/10.1016/j.jnn.2020.11.005.
Google Scholar
Kara S, Tan S, Aldemir S, Yılmaz A, Tatlı M, Dilmen U. Investigation of perceived social support in mothers of infants hospitalized in neonatal Intensive Care Unit. Hippokratia. 2013;17:130–5.
Google Scholar
Chakraborty H, Gu H. A mixed model approach for intent-to-treat analysis in longitudinal clinical trials with missing values. New York, NY: RTI Press; 2009.
Morris TH. Transformative learning through mindfulness: exploring the mechanism of change. Aust J Adult Learn. 2020;60:44–65. https://doi.org/10.3316/informit.228757006763373.
Google Scholar
Kabat-Zinn J. Wherever you go, there you are: mindfulness meditation in everyday life, 10th anniversary ed. New York, NY: Hatchette Books; 2014.
Stacey S, Osborn M, Salkovskis P. Life is a rollercoaster…What helps parents cope with the Neonatal Intensive Care Unit (NICU)? J Neonatal Nurs. 2015;21:136–41. https://doi.org/10.1016/j.jnn.2015.04.006.
Google Scholar
Grieb SM, McAtee H, Sibinga E, Mendelson T. Exploring the influence of a mindfulness intervention on the experiences of mothers with infants in neonatal intensive care units. Mindfulness. 2023;14:218–29. https://doi.org/10.1007/s12671-022-02060-w.
Google Scholar
Ginsberg KH, Alsweiler J, Alyami M, Serlachius A. Mindfulness and relaxation-based interventions to reduce parental stress, anxiety and/or depressive symptoms in the neonatal intensive care unit: a systematic review. J Clin Psychol Med Settings. 2023;30:387–402. https://doi.org/10.1007/s10880-022-09902-8.
Google Scholar
Roque ATF, Lasiuk GC, Radünz V, Hegadoren K. Scoping review of the mental health of parents of infants in the NICU. J Obstet Gynecol Neonatal Nurs. 2017;46:576–87. https://doi.org/10.1016/j.jogn.2017.02.005.
Google Scholar
Abbo Bacia J. Holistic approaches to stress management: understanding, prevention, and coping strategies. 2024. Accessed December 8, 2025.
link







